Our Treatments
At Beijing BioTech, we are committed to advancing medical science through the development and delivery of innovative, cutting-edge therapies. Our mission is to provide transformative treatment solutions that address complex and life-threatening diseases with precision and care.
We don’t just focus on treatment—we focus on redefining possibilities in healthcare. Through scientific excellence and patient-centered innovation, we strive to improve outcomes, extend lives, and create meaningful impact. Below is an overview of the pioneering therapies we proudly offer.
What is CAR-NK Therapy?
CAR-NK therapy uses genetically engineered natural killer cells to target specific cancer markers in leukemia or lymphoma.
Delivered in China for advanced cancer treatment (including Beijing, Shanghai, Guangzhou, and Chengdu), this guide covers international eligibility, infusion timelines, GMP standards, success rates, costs, and clinical trials—explaining how Beijing Biotech coordinates your complete care.
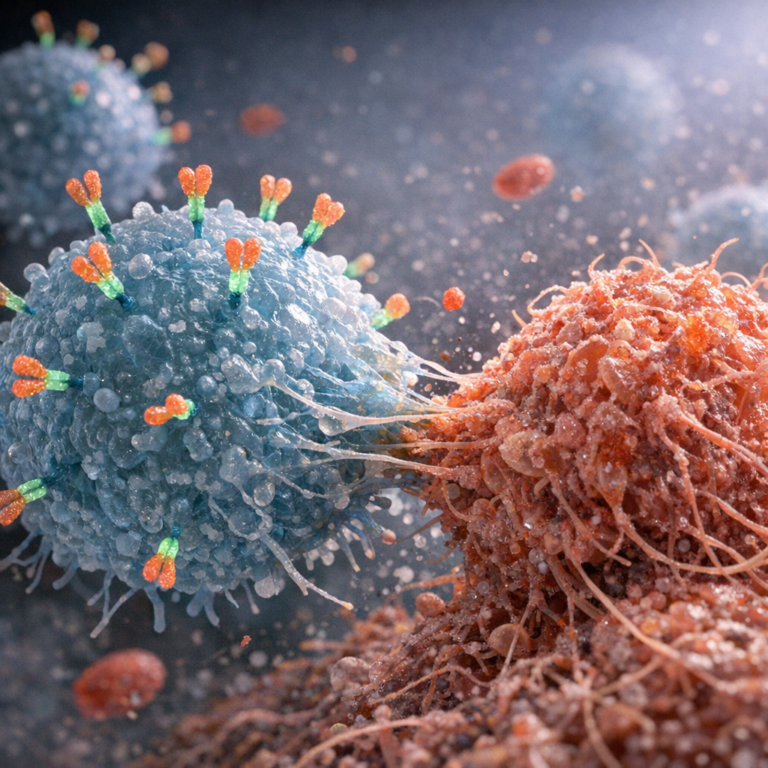
Why patients and clinicians are interested in CAR-NK:
Targeted recognition: the CAR directs NK cells toward a specific cancer marker.
Potential safety differences vs CAR-T: early studies indicate varying rates of cytokine-related toxicities, though careful monitoring remains essential.
Key point: CAR-NK is still an evolving field. In many cases, it is investigational and available primarily through clinical trials or specialized hospital programs.
NK Cell Therapy
Delivered in China for advanced cancer treatments, including options in: Beijing, Shanghai, Guangzhou, and Chengdu.
This guide explains the eligibility criteria for international patients, NK cell infusion timelines and processes, GMP manufacturing standards, and how to interpret CAR-NK success rates and safety data.
Explore CAR-NK vs CAR-T comparisons, potential side effects, hospital options in Beijing, cost and price factors, and available clinical trials for leukemia and B-cell lymphoma—while understanding how Beijing Biotech coordinates care from consultation to treatment completion.
What is NK Cell Therapy?
Natural Killer (NK) cells are part of the immune system’s “first response” team. They can recognize stressed or abnormal cells and help destroy them—sometimes without requiring a perfect match to a specific target.
In NK Cell Therapy, NK cells are collected from the patient or from a qualified donor, prepared and expanded or activated in a controlled laboratory process, and then administered back to the patient—most often by intravenous infusion. In cancer care, NK cell therapy is generally considered a form of cellular immunotherapy (a type of immunotherapy).
CAR-NK vs CAR-T
Both CAR-NK and CAR-T Therapy are targeted Immunotherapy approaches. The best choice depends on diagnosis, prior treatments, urgency, and what a qualified center can safely deliver.
| Comparison | CAR-T Therapy | CAR-NK Therapy |
|---|---|---|
| Immune Cell Used | T cell | NK cell |
| Typical Focus | More mature in several hematologic cancers (varies by country/label) | Emerging; many programs are investigational |
| Safety Monitoring | CRS and neurotoxicity (ICANS) are well-recognized and require specialized monitoring | Reactions and immune activation can occur; experienced monitoring still required |
| Typical Programs | Widely used and studied in leukemia and lymphoma | Often studied in leukemia and lymphoma programs |
| Cell Source | Often patient-derived; donor approaches vary by program | Patient or donor (program-dependent) |
| Practical Planning | Autologous manufacturing can take time; bridging therapy may be needed | Timeline depends on protocol and cell source |
How NK/CAR-NK may fit with other modalities
Some patients consider cellular therapy alongside other modalities:
- Proton Therapy for local tumor control in certain solid tumors (case-dependent)
- Targeted Therapy when a tumor has actionable markers
- Immunotherapy (e.g., checkpoint inhibitors) in selected settings
These approaches may be sequenced or coordinated – but they are not automatically combined.
A multidisciplinary team should evaluate timing, safety, and evidence for your specific case.